|
|
||||
| Home | About Us | Testimonials | Contact Us | Our Services |
|
|
||||
FibroidsFibroids are non-cancerous growths that develop in or around the womb (uterus).
Many women are unaware they have fibroids because they don't have any symptoms. Women who do have symptoms (around one in three) may experience:
In rare cases, further complications caused by fibroids can affect pregnancy or cause fertility problems. Some women with very large fibroids may have difficulty in getting pregnant whereas some may be advised to have their fibroids removed before having assisted conception or fertility treatment. Fibroids can grow anywhere in the womb and vary in size considerably. Some can be the size of a pea, whereas others can be the size of a melon. The main types of fibroids are:
Fibroid Treatment OptionsTreatment may not be necessary if you have fibroids but don't have any symptoms, or if you only have minor symptoms that aren't significantly affecting your everyday activities. Fibroids often shrink after the menopause, and your symptoms will usually either ease or disappear completely. The various treatments for fibroids are outlined below. Medication for symptoms: Medicines are available that can be used to reduce heavy periods, but they can be less effective the larger your fibroids are. These medications are described below. Levonorgestrel intrauterine system (LNG-IUS) The levonorgestrel intrauterine system (LNG-IUS) is a small, plastic, t-shaped device placed in your womb that slowly releases the progestogen hormone levonorgestrel. It stops your womb lining growing quickly, so it's thinner and your bleeding becomes lighter. Tranexamic acid Tranexamic acid tablets are taken three or four times a day during your period for up to four days. Treatment should be stopped if your symptoms haven't improved within three months. Tranexamic acid tablets aren't a form of contraception and won't affect your chances of becoming pregnant. Anti-inflammatory medicines Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and mefenamic acid, can be taken three times a day from the first day of your period until bleeding stops or reduces to manageable levels. NSAIDs work by reducing your body's
production of a hormone-like substance called prostaglandin,
which is linked to heavy periods. The contraceptive pill The contraceptive pill is a popular method of contraception that
stops an egg being released from the ovaries to prevent
pregnancy. Oral progestogen Oral progestogen is synthetic (man-made) progesterone (one of the female sex hormones) that can help reduce heavy periods. It's usually taken as a daily tablet from days five to 26 of your menstrual cycle, counting the first day of your period as day one. Oral progestogen works by preventing the womb lining growing quickly. It's not a form of contraception, but it can reduce your chances of conceiving while you're taking it. The side effects of oral progestogen can be unpleasant and include weight gain, breast tenderness and short-term acne. Injected progestogen Progestogen is also available as an injection to treat heavy periods. It works by preventing the lining of your womb growing quickly. This form of progestogen can be injected once every 12 weeks for as long as treatment is required. Common side effects of injected progestogen include:
Injected progestogen also acts as a contraceptive. It doesn't prevent you becoming pregnant after you stop using it, although there may be a significant delay (up to 12 months) after you stop taking it before you're able to get pregnant. Medication to shrink fibroids:1. Gonadotropin releasing hormone analogues (GnRHas) If you're still experiencing symptoms related to fibroids despite treatment with the above medications, your GP can refer you to a gynaecologist. They may prescribe medication called gonadotropin releasing hormone analogues (GnRHas) to help shrink your fibroids. GnRHa medications, such as goserelin acetate, are hormones that are given by injection. They work by affecting the pituitary gland which stops the ovaries producing oestrogen. The pituitary gland is a small, pea-sized gland located at the bottom of the brain. It controls a number of important hormone glands within the body. GnRHas stop your menstrual cycle (period), but aren't a form of contraception. They don't affect your chances of becoming pregnant after you stop using them. GnRHas can cause a number of menopause-like side effects, including:
2. Ulipristal acetate Ulipristal acetate is a new method of treating fibroids that have moderate to severe symptoms. It’s only recommended for women over 18 years of age. The treatment involves taking one tablet orally (by mouth) once a day, with a course of treatment lasting up to three months. During this time you shouldn't bleed and your fibroids will shrink. Surgery:Surgery to remove your fibroids may be considered if your symptoms are particularly severe and medication has been ineffective. The main surgical procedures used to treat fibroids are outlined below. 1. Hysterectomy A hysterectomy is a surgical procedure to remove the womb. It's the most effective way of preventing fibroids coming back. A hysterectomy may be recommended if you have large fibroids or severe bleeding and you don't wish to have any more children. There are a number of different ways a hysterectomy can be carried out, including through the vagina or through a number of small incisions in your abdomen (tummy). 2. Myomectomy A myomectomy is surgery to remove the fibroids from the wall of your womb. It may be considered as an alternative to a hysterectomy if you still would like to have children. However, a myomectomy isn't suitable for all types of fibroid. Your gynaecologist can tell you whether the procedure is suitable for you based on factors such as the size, number and position of your fibroids. Depending on the size and position of your fibroids, a myomectomy may involve making either a number of small incisions (cuts) in your tummy (keyhole surgery) or a single larger incision (open surgery). Myomectomies are carried out under general anaesthetic, and you'll usually need to stay in hospital for a few days afterwards. After having a myomectomy, you'll be advised to rest for several weeks while you recover. Myomectomies are usually an effective treatment for fibroids, although there's a chance the fibroids will grow back and further surgery will be needed. For further information regarding myomectomy surgery please read the information leaflet. 3. Hysteroscopic resection of fibroids A hysteroscopic resection of fibroids is a procedure where a thin telescope (hysteroscope) and small surgical instruments are used to remove fibroids. The procedure can be used to remove fibroids from inside the womb (submucosal fibroids), and is suitable for women who want to have children in the future. No incisions are needed because the hysteroscope is inserted through the vagina and into the womb through the entrance to the womb (cervix). A number of insertions are needed to ensure that as much fibroid tissue as possible is removed. The procedure is often carried out under general anaesthetic, although local anaesthetic may also be used. You can usually go home on the same day as the procedure. After the procedure you may experience stomach cramps, but they should only last a few hours. There may also be a small amount of vaginal bleeding, which should stop within a few weeks. Non-surgical procedures:As well as traditional surgical techniques to treat fibroids, non-surgical treatments are also available. These are outlined below. 1. Uterine artery embolisation (UAE) Uterine artery embolisation (UAE) is an alternative procedure to a hysterectomy or myomectomy for treating fibroids. It may be recommended for women with large fibroids. UAE is carried out by a radiologist (a specialist doctor who interprets X-rays and scans). It involves blocking the blood vessels that supply the fibroids, causing them to shrink. During the procedure, a special solution is injected through a small tube (catheter), which is guided by X-ray through a blood vessel in your leg. It's carried out under local anaesthetic, so you'll be awake but the area being treated will be numbed. You'll usually need to stay in hospital a day or two after having UAE. When you leave hospital, you'll be advised to rest for one to two weeks. Although it's possible to have a successful pregnancy after having UAE, the overall effects of the procedure on fertility and pregnancy are uncertain. It should therefore only be carried out after you've discussed the potential risks, benefits and uncertainties with your doctor. 2. MRI-guided procedures There are also two relatively new techniques for treating fibroids that use magnetic resonance imaging (MRI). They are:
These techniques use MRI to guide small needles into the centre of the fibroid being targeted. Laser energy or ultrasound energy is passed through the needles to destroy the fibroid. These treatment methods can't be used to treat all types of fibroids, and the long-term benefits and risks are unknown. As these procedures are relatively new, they're not yet widely available in the UK. Research is still being carried out, but there's some evidence to suggest that these non-invasive procedures have short- to medium-term benefits when performed by an experienced clinician. However, the effects on pregnancy and women who want to have a baby in the future aren't fully known, so this should be taken into consideration. For further information regarding your choices for fibroids:
|
| Privacy Policy | Disclaimer |
| © Copyright Berkshire Gynaecology Ltd 2025. All Rights Reserved. | Site by Visual Productions Ltd |
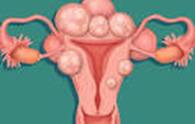 The growths are made up of muscle and fibrous tissue and vary
in size. They're sometimes known as uterine myomas or
leiomyomas.
The growths are made up of muscle and fibrous tissue and vary
in size. They're sometimes known as uterine myomas or
leiomyomas.